Gout
Overview
Gout is a common and complex form of arthritis that can affect anyone. It's characterized by sudden, severe attacks of pain, swelling, redness and tenderness in one or more joints, most often in the big toe.
An attack of gout can occur suddenly, often waking you up in the middle of the night with the sensation that your big toe is on fire. The affected joint is hot, swollen and so tender that even the weight of the bedsheet on it may seem intolerable.
Gout symptoms may come and go, but there are ways to manage symptoms and prevent flares.
Symptoms
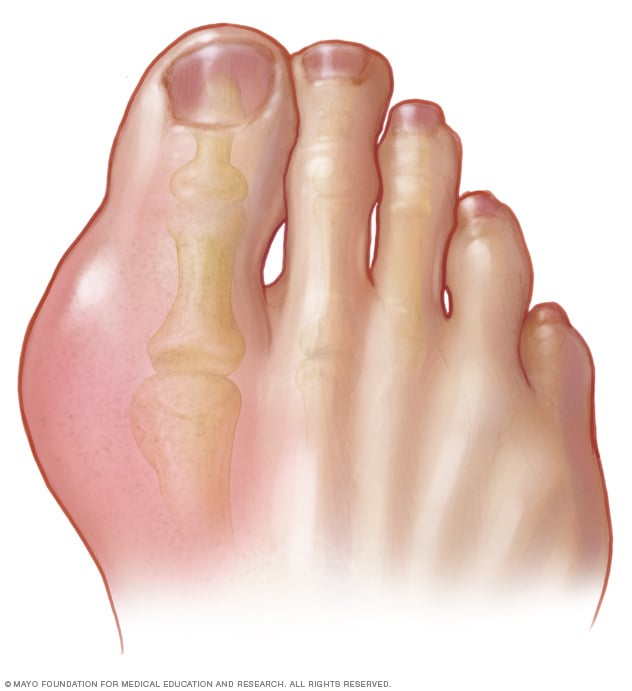
The signs and symptoms of gout almost always occur suddenly, and often at night. They include:
- Intense joint pain. Gout usually affects the big toe, but it can occur in any joint. Other commonly affected joints include the ankles, knees, elbows, wrists and fingers. The pain is likely to be most severe within the first four to 12 hours after it begins.
- Lingering discomfort. After the most severe pain subsides, some joint discomfort may last from a few days to a few weeks. Later attacks are likely to last longer and affect more joints.
- Inflammation and redness. The affected joint or joints become swollen, tender, warm and red.
- Limited range of motion. As gout progresses, you may not be able to move your joints normally.
When to see a doctor
If you experience sudden, intense pain in a joint, call your doctor. Gout that goes untreated can lead to worsening pain and joint damage. Seek medical care immediately if you have a fever and a joint is hot and inflamed, which can be a sign of infection.
Causes
Gout occurs when urate crystals accumulate in your joint, causing the inflammation and intense pain of a gout attack. Urate crystals can form when you have high levels of uric acid in your blood. Your body produces uric acid when it breaks down purines — substances that are found naturally in your body.
Purines are also found in certain foods, including red meat and organ meats, such as liver. Purine-rich seafood includes anchovies, sardines, mussels, scallops, trout and tuna. Alcoholic beverages, especially beer, and drinks sweetened with fruit sugar (fructose) promote higher levels of uric acid.
Normally, uric acid dissolves in your blood and passes through your kidneys into your urine. But sometimes either your body produces too much uric acid or your kidneys excrete too little uric acid. When this happens, uric acid can build up, forming sharp, needlelike urate crystals in a joint or surrounding tissue that cause pain, inflammation and swelling.
Risk factors
You're more likely to develop gout if you have high levels of uric acid in your body. Factors that increase the uric acid level in your body include:
- Diet. Eating a diet rich in red meat and shellfish and drinking beverages sweetened with fruit sugar (fructose) increase levels of uric acid, which increase your risk of gout. Alcohol consumption, especially of beer, also increases the risk of gout.
- Weight. If you're overweight, your body produces more uric acid and your kidneys have a more difficult time eliminating uric acid.
- Medical conditions. Certain diseases and conditions increase your risk of gout. These include untreated high blood pressure and chronic conditions such as diabetes, obesity, metabolic syndrome, and heart and kidney diseases.
- Certain medications. Low-dose aspirin and some medications used to control hypertension — including thiazide diuretics, angiotensin-converting enzyme (ACE) inhibitors and beta blockers — also can increase uric acid levels. So can the use of anti-rejection drugs prescribed for people who have undergone an organ transplant.
- Family history of gout. If other members of your family have had gout, you're more likely to develop the disease.
- Age and sex. Gout occurs more often in men, primarily because women tend to have lower uric acid levels. After menopause, however, women's uric acid levels approach those of men. Men are also more likely to develop gout earlier — usually between the ages of 30 and 50 — whereas women generally develop signs and symptoms after menopause.
- Recent surgery or trauma. Experiencing recent surgery or trauma can sometimes trigger a gout attack. In some people, receiving a vaccination can trigger a gout flare.
Complications
People with gout can develop more-severe conditions, such as:
- Recurrent gout. Some people may never experience gout signs and symptoms again. Others may experience gout several times each year. Medications may help prevent gout attacks in people with recurrent gout. If left untreated, gout can cause erosion and destruction of a joint.
- Advanced gout. Untreated gout may cause deposits of urate crystals to form under the skin in nodules called tophi (TOE-fie). Tophi can develop in several areas, such as your fingers, hands, feet, elbows or Achilles tendons along the backs of your ankles. Tophi usually aren't painful, but they can become swollen and tender during gout attacks.
- Kidney stones. Urate crystals may collect in the urinary tracts of people with gout, causing kidney stones. Medications can help reduce the risk of kidney stones.
Diagnosis
Doctors usually diagnose gout based on your symptoms and the appearance of the affected joint. Tests to help diagnose gout may include:
- Joint fluid test. Your doctor may use a needle to draw fluid from your affected joint. Urate crystals may be visible when the fluid is examined under a microscope.
- Blood test. Your doctor may recommend a blood test to measure the levels of uric acid in your blood. Blood test results can be misleading, though. Some people have high uric acid levels, but never experience gout. And some people have signs and symptoms of gout, but don't have unusual levels of uric acid in their blood.
- X-ray imaging. Joint X-rays can be helpful to rule out other causes of joint inflammation.
- Ultrasound. This test uses sound waves to detect urate crystals in joints or in tophi.
- Dual-energy computerized tomography (DECT). This test combines X-ray images taken from many different angles to visualize urate crystals in joints.
Treatment
Gout medications are available in two types and focus on two different problems. The first type helps reduce the inflammation and pain associated with gout attacks. The second type works to prevent gout complications by lowering the amount of uric acid in your blood.
Which type of medication is right for you depends on the frequency and severity of your symptoms, along with any other health problems you may have.
Medications to treat gout attacks
Drugs used to treat gout flares and prevent future attacks include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs). NSAIDs include over-the-counter options such as ibuprofen (Advil, Motrin IB, others) and naproxen sodium (Aleve), as well as more-powerful prescription NSAIDs such as indomethacin (Indocin, Tivorbex) or celecoxib (Celebrex). NSAIDs carry risks of stomach pain, bleeding and ulcers.
- Colchicine. Your doctor may recommend colchicine (Colcrys, Gloperba, Mitigare), an anti-inflammatory drug that effectively reduces gout pain. The drug's effectiveness may be offset, however, by side effects such as nausea, vomiting and diarrhea.
- Corticosteroids. Corticosteroid medications, such as prednisone, may control gout inflammation and pain. Corticosteroids may be in pill form, or they can be injected into your joint. Side effects of corticosteroids may include mood changes, increased blood sugar levels and elevated blood pressure.
Medications to prevent gout complications
If you experience several gout attacks each year, or if your gout attacks are less frequent but particularly painful, your doctor may recommend medication to reduce your risk of gout-related complications. If you already have evidence of damage from gout on joint X-rays, or you have tophi, chronic kidney disease or kidney stones, medications to lower your body's level of uric acid may be recommended.
- Medications that block uric acid production. Drugs such as allopurinol (Aloprim, Lopurin, Zyloprim) and febuxostat (Uloric) help limit the amount of uric acid your body makes. Side effects of allopurinol include fever, rash, hepatitis and kidney problems. Febuxostat side effects include rash, nausea and reduced liver function. Febuxostat also may increase the risk of heart-related death.
- Medications that improve uric acid removal. Drugs such as probenecid (Probalan) help improve your kidneys' ability to remove uric acid from your body. Side effects include a rash, stomach pain and kidney stones.
Lifestyle and home remedies
Medications are often the most effective way to treat gout attacks and prevent recurrent symptom flares. However, lifestyle choices also are important, and you may want to:
- Choose healthier beverages. Limit alcoholic beverages and drinks sweetened with fruit sugar (fructose). Instead, drink plenty of nonalcoholic beverages, especially water.
- Avoid foods high in purines. Red meat and organ meats, such as liver, are especially high in purines. Purine-rich seafood includes anchovies, sardines, mussels, scallops, trout and tuna. Low-fat dairy products may be a better source of protein for people prone to gout.
- Exercise regularly and lose weight. Keeping your body at a healthy weight reduces your risk of gout. Choose low-impact activities such as walking, bicycling and swimming — which are easier on your joints.
Preparing for an appointment
Make an appointment with your doctor if you have symptoms that are common to gout. After an initial examination, your doctor may refer you to a specialist in the diagnosis and treatment of arthritis and other inflammatory joint conditions (rheumatologist).
Here's some information to help you get ready for your appointment, and what to expect from your doctor.
What you can do
- Write down your symptoms, including when they started and how often they occur.
- Note important personal information, such as any recent changes or major stressors in your life.
- Make a list of your key medical information, including any other conditions for which you're being treated and the names of any medications, vitamins or supplements you're taking. Your doctor will also want to know if you have any family history of gout.
- Take a family member or friend along, if possible. Sometimes it can be difficult to remember all the information provided to you during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your doctor. Creating your list of questions in advance can help you make the most of your time with your doctor.
Questions to ask the doctor at the initial appointment include:
- What are the possible causes of my symptoms or condition?
- What tests do you recommend?
- Are there any treatments or lifestyle changes that might help my symptoms now?
- Should I see a specialist?
Questions to ask if you're referred to a rheumatologist include:
- What are the possible side effects of the drugs you're prescribing?
- How soon after beginning treatment should my symptoms start to improve?
- Do I need to take medications long term?
- I have these other health conditions. How can I best manage them together?
- Do you recommend any changes to my diet?
- Is it safe for me to drink alcohol?
- Are there any handouts or websites that you'd recommend for me to learn more about my condition?
If any additional questions occur to you during your medical appointments, don't hesitate to ask.
What to expect from your doctor
Your doctor is likely to ask you a number of questions. Being ready to answer them may reserve time to go over any points you want to talk about in-depth. Your doctor may ask:
- What are your symptoms?
- When did you first experience these symptoms?
- Do your symptoms come and go? How often?
- Does anything in particular seem to trigger your symptoms, such as certain foods or physical or emotional stress?
- Are you being treated for any other medical conditions?
- What medications are you currently taking, including over-the-counter and prescription drugs as well as vitamins and supplements?
- Do any of your first-degree relatives — such as a parent or sibling — have a history of gout?
- What do you eat in a typical day?
- Do you drink alcohol? If so, how much and how often?



